The Surge in Screening: Tracking the Reasons
Key policy and medical advances have converged to improve hepatitis C screening rates in Colorado and across the nation.
A new test makes screening quicker and easier; a dozen new medications make treatment more effective — and much cheaper. Federal and state governments are recommending that health care providers expand testing, and hepatitis C screening often accompanies treatment for the increasing number of people who inject drugs.
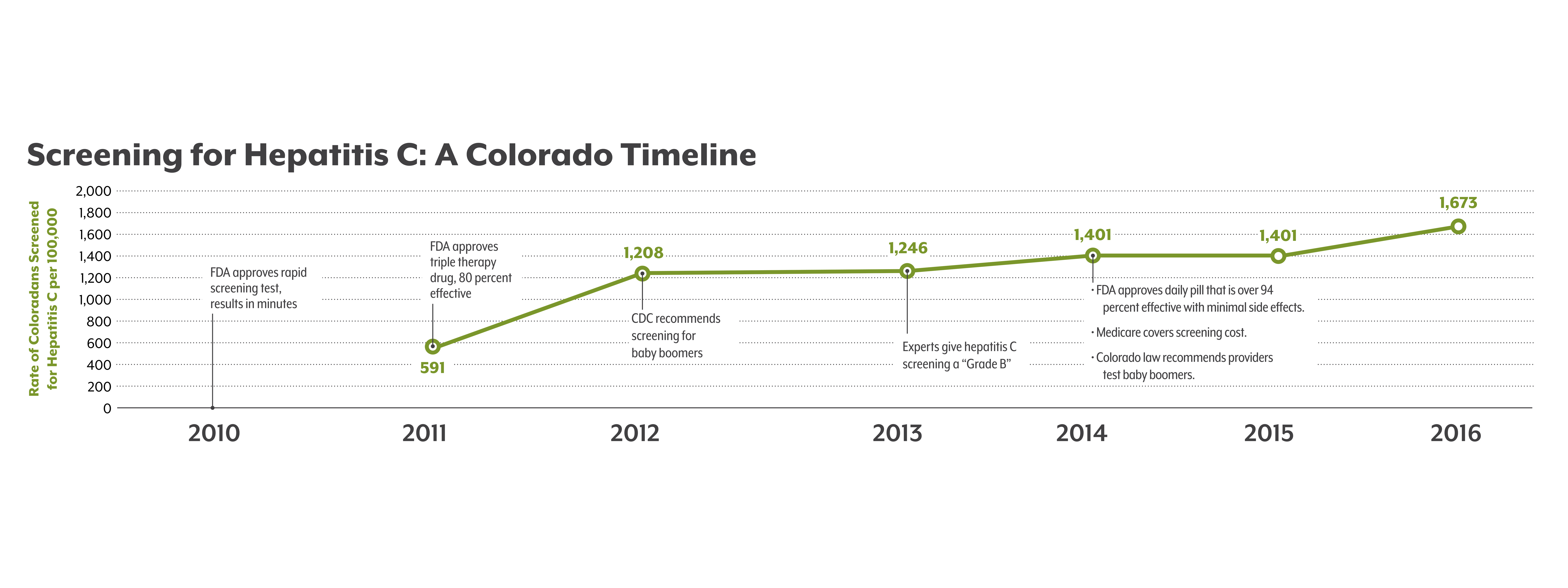
A timeline of hepatitis C screening in Colorado shows the connection between the climb in screening rates and the medical advances and policy changes occurring at the same time. (See Figure 3.)
The changes over these years include:
Medical Advances
1. Rapid Hepatitis C Test
The U.S. Food and Drug Administration (FDA) in 2010 authorized a “rapid” finger prick test that provides accurate results in 20 to 30 minutes. Most screening before that required a trip to the provider’s office so that blood could be drawn, and a weekslong wait for results.
2. Availability of New Drugs
The FDA approved a triple therapy drug— a three-medication combination — in 2011 that proved 80 percent effective at curing hepatitis C with few side effects.4
Three years later, a daily pill that is even more effective arrived on the scene. An eight-week to 12-week course of treatment has a cure rate of 94 percent.5
3. Falling Prices
Prices for hepatitis C drugs were historically astronomical — upwards of $55,000 to $95,000 for a full course of treatment. A new drug approved by the FDA in late 2017 comes in at $26,400, a fraction of the cost, and some patients and insurers negotiate even lower prices.6
A Changing Policy Landscape
1. Screening of Baby Boomers
The CDC updated its screening guidelines in 2012 to recommend that everyone born between 1945 and 1965 be screened at least once.
2. A Seal of Approval
The U. S. Preventive Services Task Force — a national panel of experts that issues widely followed recommendations for preventive services — issued a grade of “B” in 2013 for hepatitis C screening of injection drug users, indicating there was good evidence that the service would be a benefit. The task force also recommended screening the baby boomer age group.
3. A New Colorado Law
A Colorado law recommending that primary health care providers offer hepatitis C screening to each patient born between 1945 and 1965 and refer for treatment those with positive test results passed in May 2014. Within two years, by 2016, screening rates for adults in that age group increased by nearly 50 percent, according to CHI’s analysis of the APCD data.
4. Medicare Covers Screening
Medicare announced in June 2014 that it would cover the cost of screening for its clients, including the all-important baby boomer cohort.
The Opioid Epidemic
1. Screening Injection Drug Users
The increase in the number of people injecting opioids and heroin — a leading cause of hepatitis C — has driven a corresponding increase in hepatitis C testing. Injection drug users accounted for more than half of new hepatitis C cases in 2016, according to CDPHE. Generally, if someone seeks treatment for substance misuse, their provider screens for hepatitis C.
Colorado Expands Hepatitis C Treatment in Public Programs
While screening for hepatitis C is climbing across Colorado, a lawsuit has spurred increased treatment of hepatitis C by the state.
The Department of Health Care Policy and Financing (HCPF), which manages Medicaid in Colorado, in January extended access to hepatitis C treatment to all members. Previously, it had limited treatment coverage to those with the most serious liver damage, stages 2 through stage 4. This puts Colorado in line with 22 other states and territories with no restrictions.
HCPF also updated its preferred hepatitis C drug list, adding a lower-cost drug that costs about $26,000 per course of treatment compared with a drug that costs about $80,000. HCPF estimates this will reduce the average cost per enrollee from more than $80,000 to around $45,000.7
About 808 Medicaid enrollees will complete treatment in the first six months of 2018 compared with 673 if there had been no policy change, HCPF estimates.8 But even though more will be treated, the total cost will drop to $19.9 million in fiscal year (FY) 2018-19 from $24.1 million in FY 2017-18.
The Colorado Department of Corrections (DOC), meanwhile, received an additional $16.5 million for FY 2018-19 to treat inmates with hepatitis C, bringing its hepatitis C treatment budget to $20.5 million. The DOC told lawmakers it expects to treat about 784 inmates, up from 45 in 2016-17. The state estimates that 2,242 inmates have hepatitis C.9
Both moves came after the American Civil Liberties Union of Colorado sued to remove the restrictions on hepatitis C treatment.
Meanwhile, lawmakers in Colorado and across the nation are examining policies that could push hepatitis C screening rates even higher.
A bill introduced during Colorado’s 2018 legislative session would have allowed hospitals to offer sterile syringes to injection drug users, assisted schools in administering naloxone, an overdose antidote, and created a supervised injection facility pilot program in Denver where drug users could inject drugs under the supervision of people with medical training. The bill failed on a 3-2 vote in a Senate committee.
At the federal level, Congress is considering a bill that connects the dots between hepatitis C and the opioid crisis. The Eliminating Opioid-Related Infectious Diseases Act would fund work by the CDC and states to gather more data on the relationship between HIV and hepatitis C associated with injection drug use.
Conclusion
Colorado is doing a better job of screening people for hepatitis C, a good first step in getting treatment.
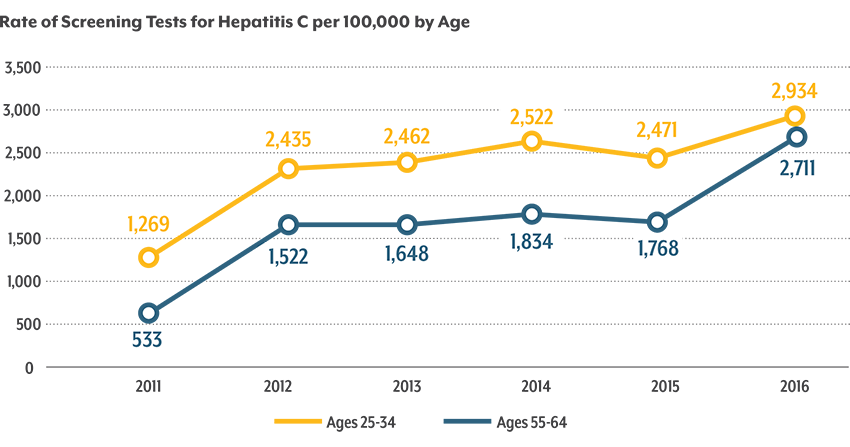
CHI’s analysis shows that Coloradans are getting screened for hepatitis C nearly three times more than in 2011 — with more people getting screened every year. While Coloradans of all ages experienced increases in screening, young adults ages 25- to 34-years-old and baby boomers ages 55- to 64-years-old had the highest rates in 2016.
While most areas of the state saw increases in screening, southeast Colorado and the Front Range experienced the biggest booms. At the same time, a handful of rural counties experienced a decrease in screening, possibly warranting for increased public health attention.
But more work remains.
While we now have a better understanding of who is getting tested and where, further research is needed to identify whether Coloradans with hepatitis C are getting the treatment they need.
Bottom line: Increased screening for hepatitis C and linking people to care can save lives.