Direct Primary Care Questions for Colorado
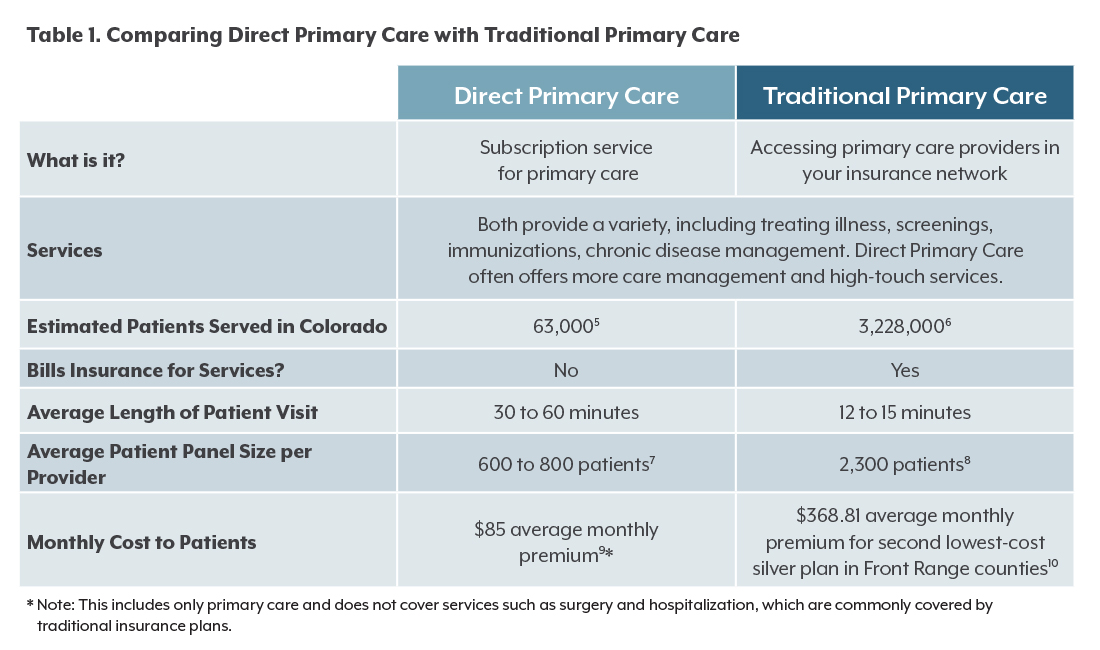
The Direct Primary Care model of health care could have benefits for Coloradans and their health care providers — from longer, richer visits to reduced red tape. But those benefits could come at a price. Opponents are concerned that Direct Primary Care could undercut traditional health care providers and make it more difficult for some patients to get care.
CHI suggests these questions for policymakers to consider when it comes to Direct Primary Care:
Could Direct Primary Care improve access to primary care in Colorado?
More than 800,000 Coloradans reported in 2017 that they couldn’t get an appointment with a doctor’s office or clinic when they needed it.15 Others said they didn’t get care because the provider was too far away, they couldn’t get child care, or they couldn’t take time off work, among other reasons.
In those cases, Direct Primary Care presents an attractive alternative—for those who can afford it. The monthly fee simplifies health care costs and offers appointment and service flexibility to access care when and where a patients needs it with services like mobile clinics and house calls.
Will Direct Primary Care hurt Colorado’s health care workforce?
Critics worry that a growing number of Direct Primary Care practices could lure physicians away from offices with traditional insurance arrangements, creating new areas of shortage, especially for Medicaid enrollees.16 Because this model supports smaller patient panels, more physicians are required to see the same number of people.17
In fact, if every primary care physician in Colorado were to adopt the Direct Primary Care approach, the state would need 4,400 more physicians to make up for the smaller patient panels.18 Adoption of the model would likely never reach this level, but in a profession already facing shortages, the prospect of losing further capacity has some providers worried.19
Dr. Mark Tomasulo, founder of PeakMed, which runs a number of Direct Primary Care practices, says that while there could be a short-term impact on physician numbers, in the longer term he believes the personal and professional benefits of Direct Primary Care could reduce physician burnout, keeping them practicing longer and attracting more doctors to primary care. Swapping a high quantity of interactions for high quality interactions with patients could be a boon to primary care providers, he says.
Would it create a “two-tiered” health care system?
The departure of doctors from traditional primary care to Direct Primary Care could exacerbate disparities in access to health care based on race/ethnicity. Evidence suggests providers using a subscription model on average see fewer African-American, Hispanic or Medicaid patients.20 Medicare enrollees may also be affected, since most clinics opt out of offering to care for them due to red tape.21
Some clinics in Colorado try to address this by seeing patients who are publicly insured outside of the Direct Primary Care framework. While it is illegal for a Direct Primary Care doctor to charge a Medicaid member for services, some operators run a parallel, traditional practice that takes insurance of all types, including Medicaid and Medicare. Others say they reserve a percentage of their patient load for “charity care” and see Medicaid and uninsured patients pro-bono.
How could it affect Health First Colorado (Medicaid) enrollees?
The American Academy of Family Physicians and the Colorado Commission on Affordable Health Care have both recommended pilot programs to allow Medicaid members to use Direct Primary Care clinics.23,24 To date, no efforts have been made to allow such a program, although some physicians are expressing interest in a test run. They believe a pilot could save the state Medicaid program money by keeping Medicaid patients healthier and avoiding costly medical expenses.
Conclusion
Direct Primary Care has received a lot of attention as health care leaders consider how to fix a primary care system that often features high insurance prices, low satisfaction for both patients and providers, and less-than-optimal health results.
Ever-increasing health care costs have some wondering if Direct Primary Care could be a solution for delivering efficient primary care in Colorado. But could it leave behind at-risk populations and the clinics serving them?
It will be important for Colorado to weigh the potential outcomes.
Endnotes
1 Colorado Health Institute analysis of Colorado Direct Primary Care clinics.
2 Colorado Revised Statues Title 25.5: Health Care Policy and Financing 25.5-4-301. http://codes.findlaw.com/co/title-255-health-care-policy-and-financing/co-rev-st-sect-25-5-4-301.html
3 https://www.kevinmd.com/blog/2014/08/direct-primary-care-concierge-medicine-theyre.html
4 http://www.latimes.com/health/la-he-concierge-medicine-20170114-story.html
5 Colorado Health Institute analysis of Colorado Direct Primary Care clinics.
6 Colorado Health Access Survey, 2017.
7 Colorado Health Institute analysis of Colorado Direct Primary Care clinics.
8 Alexander GC, Kurlander J, Wynia MK. “Physicians in Retainer (“Concierge”) Practice. A National Survey of Physician, Patient, and Practice Characteristics.” Journal of General Internal Medicine, 2005;20(12):1079–1083
9 Colorado Health Institute analysis of Colorado Direct Primary Care clinics.
10 Connect for Health Colorado: Premium data for 40-year-olds, 2017
11 PR Newswire. “Paladina Health, UnitedHealthcare and State of Colorado Partner to Provide Innovative Physician-Led Primary Care to State Employees.” January 13, 2016. https://www.prnewswire.com/news-releases/paladina-health-unitedhealthcare-and-state-of-colorado-partner-to-provide-innovative-physician-led-primary-care-to-state-employees-300203491.html
12 Paladina Health. “Your Available Locations.” https://www.paladinahealth.com/clients/state-colorado. Accessed June 27, 2018.
13 https://leg.colorado.gov/bills/hb17-1115
14 https://nexterahealthcare.com/locations/
15 Colorado Health Access Survey, 2017.
16 Wu, WN et al. “A Direct Primary Care Medical Home: The Qliance Experience.” Health Affairs 36(5). (May 2017). http://content.healthaffairs.org/content/29/5/959.full?ijkey=5faaf28d6606e333829de56c2320df8d3d4f582e&keytype2=tf_ipsecsha. Accessed May 16, 2017.
17 Weisbart, E. “Is Direct Primary Care the Solution to Our Health Care Crisis?” (September-October 2013). Family Practice Management 23(5); 10-11. http://www.aafp.org/fpm/2016/0900/p10.html. Accessed May 16, 2017.
18 CHI calculated this number using CHAS data and average panel sizes for traditional and Direct Primary Care providers.
19 Robert Graham Center, Colorado: Projecting Primary Care Workforce, https://www.graham-center.org/content/dam/rgc/documents/maps-data-tools/state-collections/workforce-projections/Colorado.pdf
20 Alexander, GC et al. “Physicians in Retainer (“Concierge”) Practice. A National Survey of Physician, Patient, and Practice Characteristics.” Journal of General Internal Medicine (2005)20: 1079. https://link.springer.com/article/10.1111/j.1525-1497.2005.0233.x. Accessed May 16, 2017.
21 Eskew, PM et al. “Direct Primary Care: Practice Distribution and Cost Across the Nation.” Journal of the American Board of Family Medicine (November-December 2015) 28(6). Pages 793-801. http://www.jabfm.org/content/28/6/793.full.pdf+html. Accessed May 15, 2017.
22 Colorado Department of Health Care Policy and Financing. Policy Statement: Billing Health First Colorado Members for Services. https://www.colorado.gov/pacific/hcpf/policy-statement-billing-medicaid-members-services. Accessed May 14, 2018
23 Colorado Commission on Affordable Health Care. 2017 Final Report. June 30, 2017. https://www.colorado.gov/pacific/sites/default/files/Cost%20Commission%20November%202017%20report%20v3%20draft_1.pdf
24 Letter to Bill Lindsay, Colorado Commission on Affordable Health Care, from Tamaan Osbourne-Roberts, Colorado Academy of Family Physicians. February 24, 2017. https://www.colorado.gov/pacific/sites/default/files/CAFP_DPC%20Recommendations%20to%20Cost%20Commission%20February%202017.pdf